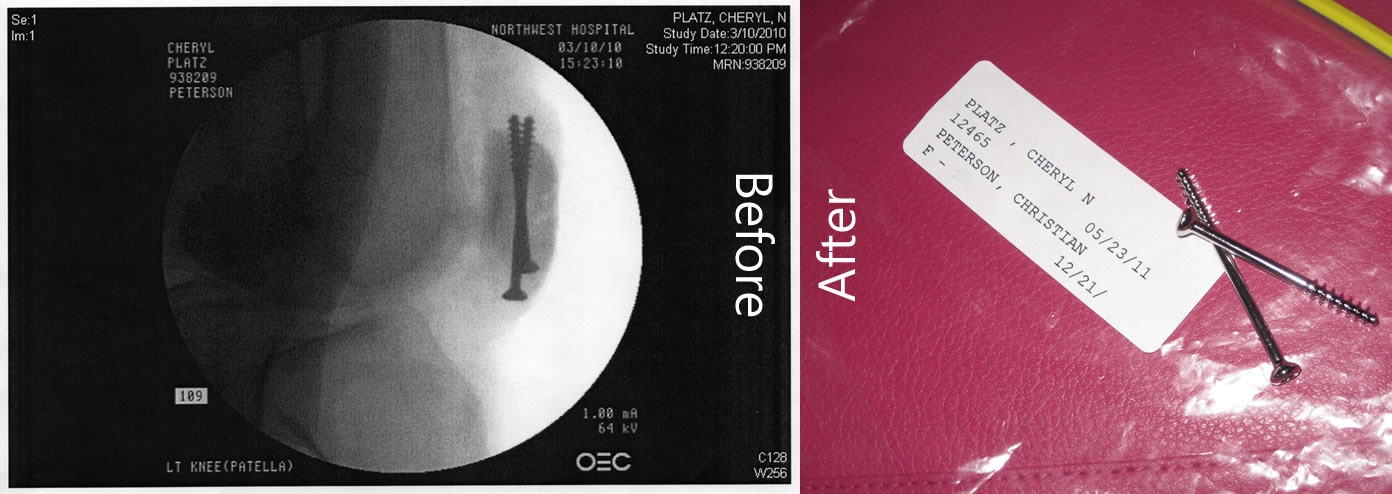
A few days ago, I had arthroscopic knee surgery to remove the two screws that have been holding my shattered kneecap together since March 10th of last year. Hopefully, by doing this, I can jumpstart a final phase of recovery and move me out of the temporarily disabled category. Over the past year or so, the prospect of getting the screws out was a light at the end of the tunnel. I talked to many folks who have had hardware in for one reason or another, and all seemed to agree that if the option to remove the hardware is available, it’s one worth pursuing. And looking at my original x-rays, I can see why – they can’t cap the pointed ends of the screws, so they look like 2 drywall screws poking my muscle tissue.
With an injury like this, you end up spending a lot of time with your medical team. I was in weekly for quite a while, evaluating progress, x-rays, and setting new goals. (I was in a Bledsoe adjustable leg brace, and each week we added another 10 degrees of flexibility.) In a way, then, this is the end of a long journey with this team, assuming recovery goes reasonably well.
Somewhere along the way, I realized that I wasn’t just a number to these doctors and nurses – perhaps because it turns out fractures like this are not common. But it was clear that they remembered me specifically, remembered my personal issues and were rooting for my recovery. In particular, Dr. Peterson’s nurse Ellie has always been upbeat and supportive. She was also in the procedure yesterday, and when she stopped by to talk to me pre-operation, she had a story for me:
We were just talking about you yesterday! We just got a new patient who shattered his patella while in Italy. They had to hardcast him and fly him back like that. His injury was like yours- he just fell. The situation reminded us of you and we were talking about your procedure today and how well you were doing!
It’s somewhat adorable to think of the nurses doting on past patients fondly. (It also makes me feel slightly less idiotic to find out I’m not the only one in the universe who can sustain such a major injury doing something as trivial as walking, though I wouldn’t wish that on anyone.) Most of my doctors seem to remember me pretty well thanks to all of my unique medical conditions. (I stopped watching House when I realized there were multiple episodes about conditions that I have lived with.) I wonder if being ‘memorable’ as a patient leads to better care long-term.
When I think about my medical care, I find it hard to say what makes a good doctor – even if you do suspect your physician treats you poorly, it’s too much of a hassle to shop around for comparison’s sake. I just read one friend’s blog complaining about her gastroenterologist who has made her cry on occasion. And with situations like my knee or my original ovarian cyst, there’s no time to pick a physician – you go with the first referral who can take you, given the urgency of the situation. That could easily turn out badly.
One thing that is very important to me in a doctor: all of my doctors have been very respectful of my illnesses and concerns. (Maybe because they know I’m terrible at being a hypochondriac – whenever I sense something is wrong, I’m usually right!) It was that respect for my concerns and my GP’s attention to detail that led to my early onset hemachromatosis diagnosis (ha! poetry) – I was halfway to liver damage when we caught it, and a few months more might have proved disasterous. My doctors have all historically been very good about taking as long as I need to discuss options or questions, and they have all worked hard to avoid invasive or disruptive tests by covering the gamut of simpler tests first.
I’m very grateful that my orthopedic surgeon – who I didn’t choose, he was a referral from the ER – used to be a physician for the Mariners and seems to be pretty good in the OR. But my friend with the gastroenterologist with terrible bedside manner – well, it’s such a hassle to get your records transferred and to establish a new physician relationship that it’s almost monopolistic! Situations like hers seem to be a compelling argument for tools like HealthVault – having access to your own medical records might empower people to find the most appropriate care.
Despite all of my experience with medical procedures, yesterday was a first for me: Dr. Peterson and his staff had a vase of get-well flowers for me at my discharge. Such a little touch, but a really nice one, especially at a key milestone in such a long journey. It makes one wonder — would such small actions, like unexpected flowers from a doctor, have any positive effect on recovery? What tricks do doctors use to keep track of their disparate patients that could be applied in other industries? I wonder what defines a “good” or “memorable” patient for doctors. Demeanor? Degree of recovery? Sense of humor? It’s also comforting when nurses stay with the same doctors long-term. It’s great to see familiar faces who don’t need to spend 40 minutes reviewing your chart to remember who you are. Does that have a measurably positive impact on recovery? In the end, the healthcare system is in desperate need of changes that pay attention to the service design, and how each interaction with disparate healthcare providers helps or hinders patients on their journeys.
As for me, I got a nice closure from “reclaiming” the surgery center yesterday. It was the same place where my original surgery took place. I remember the first time I was there – sliding into deep depression thanks to the uncertainty about my ability to ever resume the things I loved, like travel, acting, or dance. Last time, it was a huge ordeal just getting onto the operating table. This time, I was well enough that they even let me WALK into the operating room. Re-entering that room on my own terms felt like no small victory. And that feeling of triumph will no doubt help me as I try to recover from this new surgery.
Post-op, I am staying home for the first week of recovery, then taking it VERY EASY since my kneecap is hollow for the next 6 weeks or so. My entire leg is bandaged, thigh to foot, in a huge white ace bandage with enough padding to look like a kneepad in the middle. It amuses me that the ace bandage is white – normally they’re beige, so this makes me look like a cartoon character recovering from a dropped piano, or something. It’s driving me crazy that I can’t see the incisions yet, but I’m not allowed to remove the bandages for 3 days. Until then, it’s just ice, elevation, and hydrocodone.
…And yes, I did get to keep the screws.
